Chair's Column: Career Satisfaction and Work-Life Integration: Results from the 2017 Faculty Survey

Dr. Gillian Hawker

Due to sensitive nature of the questions, this most recent faculty survey was conducted anonymously and online. In brief, of the 764 full time faculty members surveyed, 414 (52%) responded (166 women and 248 men), with excellent representation by faculty demographics, hospital site, division, academic position description and rank. We therefore feel comfortable that the results we present to you here and in future newsletters have high internal validity. If you are interested in the detailed summary of our respondents, please click on the link.
For this month’s column, I want to focus on the survey results regarding career satisfaction and work-life integration. Analyses are ongoing to understand the influence of gender, race/ethnicity and religion on faculty members’ responses – these findings will be reported separately.
Career Satisfaction and Work-Life Integration
The Department of Medicine (DOM) at the University of Toronto is a dynamic, engaging, collaborative place to work, and is highly regarded in Canada and abroad. However, individual experiences vary, and there are always ways for us to support each other more effectively and create a better shared work environment.
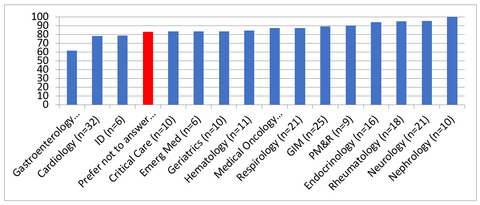
The 2017 Faculty Survey strove to understand our collective experience with career satisfaction and work-life integration. We were delighted to find that career satisfaction is high among our faculty: 88% of female and 84% of male faculty members expressed being somewhat or strongly satisfied with their careers, compared with 83% and 86%, respectively, in 2015. When examined by site, more than 75% of respondents at all sites indicated being satisfied with their careers. Results were similar when examined by division, with a majority of male and female faculty members reporting being somewhat or strongly satisfied with their careers. However, some variability in career satisfaction was noted when the results were examined by sex and division (Figure 1). High career satisfaction was reported by more than 75% of women in Gastroenterology, GIM, Geriatrics, Hematology, Infectious Diseases, Nephrology, Neurology and Rheumatology, and by more than 75% of men in Endocrinology, Nephrology, Physical Medicine and Rehabilitation.
Figure 1: Proportion that indicated somewhat or very satisfied with their career
(Note: Divisions with <= 5 respondents are excluded)
We also learned from you that we can do better to create opportunities to collaborate with others across all faculty levels, divisions/departments and health disciplines at the level of the university, hospital and research institutes, and we continue to engage in these efforts through the mandates of each of the Vice-Chairs and through our Departmental Division Directors (DDDs).
Individuals working in the academic position descriptions (APDs) of Clinician Investigator (C-I; n=64) and Clinician – Quality Improvement (C-QI; n=19) were less satisfied than those in other APDs with the amount of time they have to fulfill their scholarly obligations (% dissatisfied: CI 31% and CQI 42% versus about 20% for the other APDs). Irrespective of the APD, female respondents were more likely than their male counterparts to report dissatisfaction in meeting scholarly obligations (34% vs. 18% overall). There may be institutional barriers that contribute to these findings, which we are working on. Although we revised our APDs in 2015 to allow for three groups of individuals with varying quantity and type of scholarship in QI (CQI – 20-30% protected time; CI-QI – 40-60% protected time; CS-QI 70%+ protected time), it seems there remains confusion regarding the expectations of our QI faculty. Based on these findings, we will regroup and rethink how best to support both our CI and CQI faculty members! At the same time, we would like to encourage all faculty members to review their APD and ensure that it is the most appropriate. As careers evolve, APDs may need to be changed.
It is a privilege to work at a top academic medical center, but we know that this comes with its own pressures. Adequate work-life integration and wellness is central to our professional and personal lives. Almost 50% of faculty members indicated that their work life does not allow for sufficient personal or family time, which is a matter of great concern to me. More than 25% of respondents, irrespective of APD, felt they had insufficient personal and family time; more than 50% of individuals in C-I, C-QI, and Clinician-Scientist (C-S) APDs did not feel they have sufficient time. Over 85% of faculty members voicing an imbalance attributed it to work activities (approximately 61%) or their own personality / work style (33%), rather than personal or family activities.
Overall, the proportion of respondents reporting feeling burned out from their work was low (64% indicated never or infrequently experiencing feelings of burnout). However, compared with male faculty, female faculty were about twice as likely to report burn out (p=0.003). I was also concerned to learn that faculty members do not feel comfortable raising personal or family considerations when scheduling work obligations. More women experienced discomfort than men, and faculty members across the APDs and from most sites felt similarly. There was greater comfort in voicing personal or family matters at the Hospital (DoM 48%; Division 58%) than at the University DoM (35%) level. These issues were also raised at our recent Summit on Women in Academic Medicine and must be addressed. We are engaged in ongoing conversations with the Physicians-in-Chiefs (PICs) and DDDs about how best to build systems of clinical coverage and shared work that allows all faculty members to attain work-life integration.
Some of the richest and most useful information that we obtained from the Faculty Survey was from the qualitative feedback that you provided. First and foremost, the amount and quality of the feedback given is a testament to the high level of engagement of our faculty members.
Broadly, the comments can be grouped under a few themes:
Citizenship
- For some faculty members, low career satisfaction was attributed to favoritism, lack of collegiality and divisive leadership.
- Faculty members had concerns about voicing family or personal obligations, as well as burnout, because of the implications that this may have for career advancement.
- There was a sense that there is a lack of resiliency in the system to buffer against stressful events, and this was cited as a greater cause of burnout than the actual quantity of work.
- Many respondents emphasized the importance of mentorship.
We hear you. Here are some of the things we are working on to build a sense of citizenship across the DOM:
- We are promoting a culture shift that prioritizes equity, fairness and the “collective” rather than the individual. Consistent demonstration of professionalism and citizenship is a prerequisite for recruitment, continuing appointment and promotion for all faculty members irrespective of rank or position.
- We are undertaking regular evaluations of our leaders and providing coaching and other opportunities for leadership development as needed.
- We have outlined clear processes for recruitment and hiring, promotions and the selection of leaders and awards recipients.
- We are developing a diversity dashboard (with a working group led by Ayelet Kuper and Larry Robinson) through the Mentorship, Equity and Diversity committee.
- We have a zero-tolerance policy for unprofessional behaviour, and we have reviewed and improved our existing reporting mechanisms so that leaders at each site have the support, guidance, and resources needed to respond meaningfully.
- We have recruited Mentorship Facilitators across most divisions and are trying to ensure that everyone has a formal mentor.
- We appreciated one respondent’s suggestion to institute a mechanism for “Positive Incident Reporting,” which we agree should be incorporated on our website.
Clinical duties, including call, along with high demands of the APDs
- The clinical work within the DOM has gotten progressively busier, in terms of both volume and complexity.
- Faculty members are using evenings and weekends to work on scholarly activities.
- The high demands of the APDs were felt to be inconsistent with existing hospital pressures and growing clinical volumes and complexity, leaving insufficient time for academic work.
We hear you. Here are some of the things we are working on to improve Work-Life Integration and respond to rising patient volumes and complexity across the DOM:
- We are looking at options for flexible work hours and work sharing. This is not that simple for physicians where the ‘business day’ is poorly circumscribed, but must be tackled.
- Although the DOM does not have direct responsibility for clinical care, we are engaged with our PICs who have received the survey results and are working hard to find solutions to manage rising patient volumes and complexity that are tailored to local contexts and each division.
Transparency in Remuneration
- Faculty members feel they have to prioritize clinical work because non-clinical work is not well remunerated.
- Work stress and financial stress were cited as two competing forces that impede work-life integration.
- In Recruitment, Hiring, Promotion
- In Selection for Awards, Leadership, Committees
We hear you. Here are some of the things we are working on to increase transparency within the DOM:
- Along with the PICs and other stakeholders, we are examining models of funding as well as best practices in financial transparency.
- We have streamlined protocols and processes for recruitment, hiring and promotion, as highlighted on our DOM website. All selection committees must undertake Unconscious Bias training prior to engaging in these efforts.
- We will continue to search for strategies to ensure that all faculty members can participate in matters of governance including, for example, trying to set meeting times that accommodate personal and family obligations.
In short, while it is heartening to learn that a majority of our faculty members experience high career satisfaction, this should not blind us to the ways that we can serve our faculty, and by extension our patients, learners and community, more effectively. Although we have already taken some early steps to remedy the identified gaps, it is clear that there is still a long way to go. I am committed to creating a DOM that helps each faculty member become the best possible versions of themselves, professionally and personally. I look forward to working with all of you in this endeavor.



